7 results
Transcranial magnetic stimulation for catatonia: case series
- G. Mamedova, N. Zakharova
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1019
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Catatonia is diagnosed in 5–43% of patients with various mental disorders, thus actualizing the problem of elaborating therapeutic interventions for catatonia on an outpatient basis. Although the current experience in application of transcranial magnetic stimulation (TMS) in catatonia is limited, it provides promising data on positive effect of dorsolateral prefrontal cortex (DLPFC) stimulation in a series of clinical observations. According to the available data, TMS shows comparable efficacy with electroconvulsive therapy, but unlike it is safe and does not require general anesthesia in intensive care unit.
Objectivesto evaluate the efficacy and safety of TMS in the treatment of catatonia in patients with mental disorders
MethodsFour patients were diagnosed with catatonia as part of schizophrenia spectrum disorders in three cases (P1,4,7) and in one case within the structure of recurrent depression phase (P8). Psychopathological examination includes PANSS, SAS, NSA-4, BFCRS, NCRS, and BACS.
Personalized choice of stimulation protocol was determined by rCBF lateralization in DLPFC reflecting the neuronal activity in that region: 1) P1, P4, and P8 underwent 20 sessions of high-frequency stimulation at the frequency of 20 Hz with the amplitude of 120% MT in the projection of left DLPFC 2) P7 underwent 20 sessions of low-frequency stimulation at the frequency of 1 Hz with the amplitude of 120% MT in the projection of right DLPFC
ResultsSafety evaluation was performed daily during TMS sessions. None of participants reported any adverse events at high compliance.
The efficacy was estimated during by the following criteria: 1) positive clinical response: decline of BFCRS and NCRS scores by 70% from the primary evaluation 2) achievement symptomatic remission (total BFCRS and NCRS score 3 and less).
Positive clinical response was detected in all four patients, however, symptomatic remission was formed only in two of them (P1 and P4) referring to BFCRS.
Evaluation of neurotransmitter concentration: P1, P7, P8 showed a tendency for absolute and relative glutamate concentration values to approach normal. After the TMS course GABA concentration diminished in all cases but P4, in whom the elevation of GABA level was registered.
ConclusionsTMS potentially activates metabolic processes in brain tissues, thus promoting deceleration of pathological mechanisms and potentiating neuroplasticity with procognitive effect, expressed primarily in the increase of processing speed and response to it, as well as in the improvement of working memory. To summarize, the influence of TMS on local brain regions makes it possible to achieve a positive clinical effect in treatment of catatonia.
No strong and unequivocal results were received for the efficacy of TMS in treatment of catatonia. A positive clinical effect was seen, however, insufficient for achieving remission in the majority of subjects.
Disclosure of InterestNone Declared
EXPERIENCE OF PHARMACOGENETIC TESTING IN THE TREATMENT OF ANTIPSYCHOTICS
- M. Kaydan, N. Zakharova
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1070
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
One of the promising methods for optimizing treatment in order to achieve high-quality remissions is a personalized approach to prescribing therapy in the form of pharmacogenetic testing, the feasibility of which has already been substantiated and proven in a number of clinical guidelines. By the beginning of 2022, several influential regulatory and expert organizations recommend considering the results of genetic testing when prescribing therapy. Thus, personalization of antipsychotic therapy is being introduced in the world practice.
ObjectivesTo establish the significance of pharmacogenetic markers that determine the efficacy and safety of antipsychotic therapy in patients with schizophrenia in clinical practice.
MethodsThe study included 264 patients (141 men, 123 women; 27.3 ± 4.5 years) from among the first hospitalized in a psychiatric hospital in the period 2018-2020, meeting the inclusion criteria (psychosis within the schizophrenia spectrum disorders; consent to participate in research). Non-inclusion criteria - signs of organic brain damage; alcohol or substance abuse; somatic pathology in the stage of decompensation). The examination took place in three stages - in the first days of hospitalization at the peak of the acute condition and during the formation of remission - after 6 and 12 months. Genetic analysis was performed using high-density biochips from Illumina CoreExome Bead (Illumina Inc, USA). During the follow-up observation, some patients dropped out due to refusal to undergo examination, change of diagnosis or change of place of residence. After 6 and 12 months, it was possible to trace the dynamics of the state of 91 patients (50 men, 41 women; 24.9 ± 4.6 years).
ResultsBased on the follow-up results, two types of schizophrenia dynamics were identified - with a relatively favorable and unfavorable course. The formation of a relatively stable remission corresponding to the criteria proposed by the working group was noted in 47 patients (51.6%), carriers of gene polymorphisms: DRD2 rs1799732 (del); COMT rs4680(GG); BDNF rs6265 (CC); ANKK1 rs1800497 (GG); MC4R rs489693 (AA); ABCB1 rs1045642 and ABCC1 rs212090 (GG). An unfavorable course with the ineffectiveness of antipsychotics was found in 48.4% of cases in patients with DRD2 rs1799732 (G/del) carriers; COMT rs4680(AA); BDNF rs6265 (TT); ANKK1 rs1800497 (AA); MC4R rs489693 (GG); ABCB1 rs1045642 and ABCC1 rs212090 (AA).
ConclusionsAfter analyzing the results of genetic testing and clinical and dynamic characteristics of the course of schizophrenia, we can talk about the relationship between the establishment of high-quality remission in the presence of polymorphisms in the genotype, whose role has been proven in terms of the effectiveness and safety of antipsychotics.
Disclosure of InterestNone Declared
COVID-19-associated schizophrenia-like psychosis during the COVID-19 pandemic
- L. Bravve, N. Zakharova
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S798
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The viral theory of the development of psychoses was formulated in the 19th century, but the role of viral agents in the pathogenesis of psychoses remains a matter of debate. In the context of the 2020 pandemic, the results of several papers on the characteristics of psychotic disorders in COVID-19 have been published. Coronaviruses are neuroinvasive, capable of affecting mental and body functions.
ObjectivesThe aim of the study was to identify patients with acute psychosis without a history of mental disorders in order to test the hypothesis about the possibility of manifestation of schizophreniform psychosis due to a viral attack.
MethodsWithin a year and a half, 50 patients with mental disorders associated with COVID-19 were identified. The reason for hospitalization in a psychiatric hospital is the development of acute schizophreniform psychosis against the background of a new coronavirus infection. The diagnosis was verified according to traditional clinical criteria and modern psychometric tools. Inclusion criteria: no previous visits to a psychiatrist; verified acute polymorphic psychotic disorder and coronavirus infection COVID-19 (ICD-10); manifestation of psychosis against the background of infection with COVID-19; age 18-60 years; consent to participate in the study. Exclusion criteria: signs of organic brain damage; indications of substance abuse; delirium of any etiology; somatic pathology in the stage of decompensation.
Results27 women (54%) and 23 men (46%), aged 20 to 57 years (average age 34.5±7.6), of which 18 people (36%) worked, 2 (4%) studied , 29 (58%) people are unemployed. 27 people (54%) are single, 16 (32%) are married, 7 (14%) are divorced; 18 people (36%) were raising children, which indirectly indicated a relatively favorable premorbid functioning. At the time of the examination, the condition was determined by polymorphic psychotic symptoms with a predominance of dissociative-delusional, paraphrenic and oneiric phenomena with plots containing plots of infection and the spread of coronavirus. At the same time, the sum of PANSS is from 53 to 130 (85) points, including PANSS P - from 15 to 37 (27), PANSS N - from 7 to 44 (18), PANSS G - from 23 to 57 (39.9 ); P1 - 5.7; P3 - 5.1. When comparing the obtained data with the world experience, we found some differences. Delusional symptoms were diagnosed twice as rarely, cases with tactile hallucinations were not detected, but catatonic symptoms were observed twice as often, and manic arousal was twice as rare. In general, the studied data are comparable with the results published in the world practice.
ConclusionsThe unique experience of the coronavirus pandemic will allow us to assess the influence of environmental factors, namely the role of infections, in the manifestation or predisposition to schizophrenia spectrum disorders. It is planned to evaluate the dynamics of the course of the disorder after the relief of the acute period.
Disclosure of InterestNone Declared
Decrease in anterior cingulate cortex GABA in schizophrenia at early stage
- A. Manzhurtsev, S. Nevzorova, M. Ublinskiy, L. Mosina, I. Melnikov, G. Mamedova, V. Ushakov, N. Zakharova, M. Shlyapnikov, D. Andreyuk, T. Akhadov
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S609-S610
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is evidence that the concentrations of the main inhibitory neurotransmitter (GABA) may be altered in schizophrenia. The purpose of this study is to find the changes in the GABA concentration in the area of anterior and posterior cingulate cortex of patients with early-stage schizophrenia using the spectral-edited magnetic resonance spectroscopy.
ObjectivesTo measure the cerebral concentrations of the gamma-aminobutyric acid in schizophrenia patients at early stage.
MethodsThirty-one subject, 18 controls (11m+7f, 29.6±5.7 y.o.) and 13 schizophrenia patients (F20.0, 8m+5f, 27.5±3.1 y.o.). Philips Achieva dStream 3T MRI scanner, standard head coil. The 3D T1w head images and MEGA-PRESS GABA spectra in ACC and PCC areas were acquired with the following parameters: 50x25x25 mm, TR = 2 s, TE = 64 ms, 180-editing pulses applied at 1.9 ppm and 7.6 ppm, NSA = 288 (acq.time ~10 min). GABA spectra were processed in Gannet program. The intensities of the GABA, Glutamate+glutamine (Glx), creatine (Cr) and unsuppressed water signals were acquired. T-test was used in search for between-group differences.
ResultsIn ACC region, significant reduction of the GABA/Water was observed (by ~15%, p=0.02) as well as a trend to a decrease in GABA/Cr (by ~10%, p=0.07) in schizophrenia. In PCC, no significant GABA/Water or GABA/Cr differences were observed. Glx/Water and Glx/Cr in both areas were also unchanged.
Image:
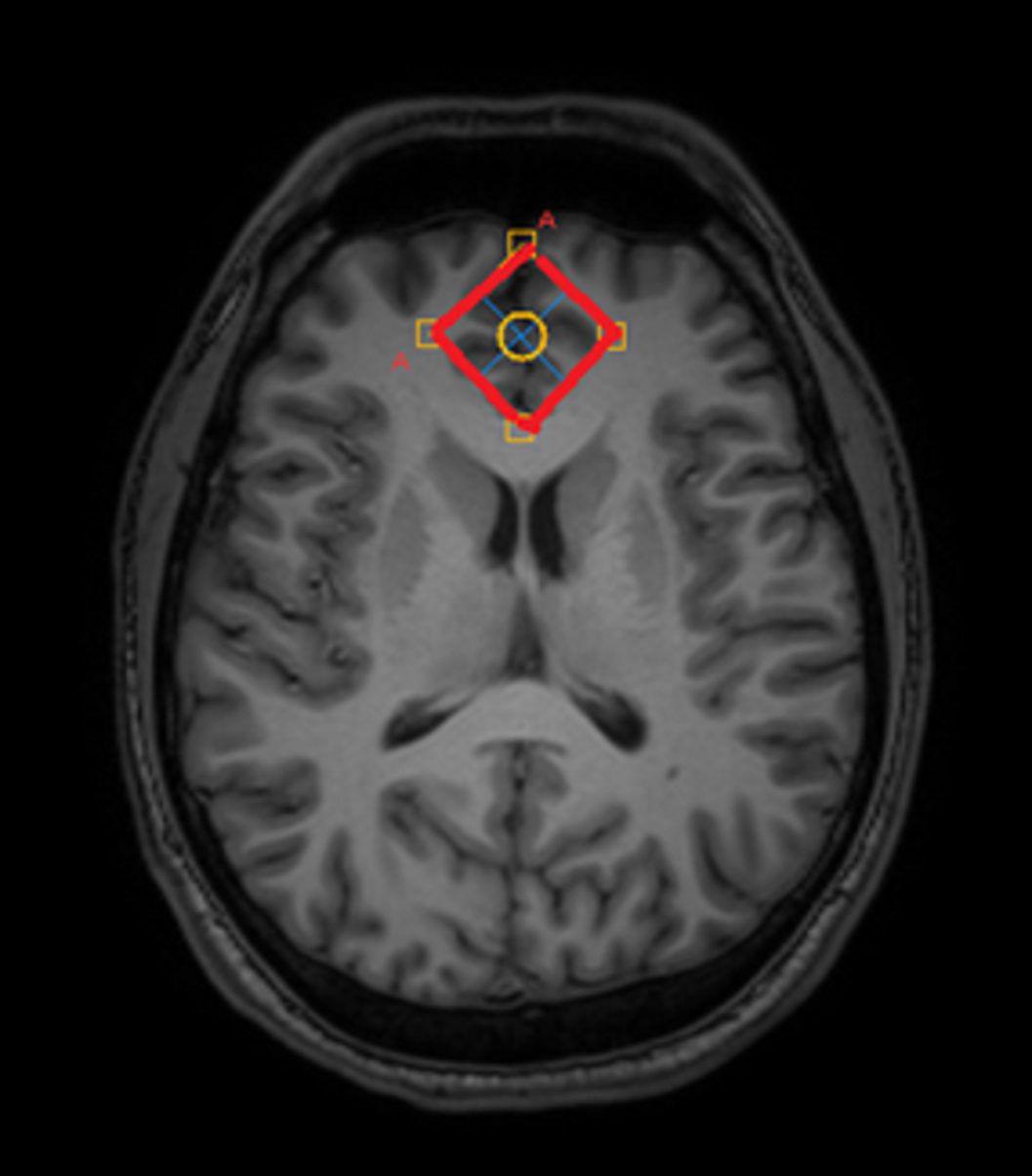
Image 2:
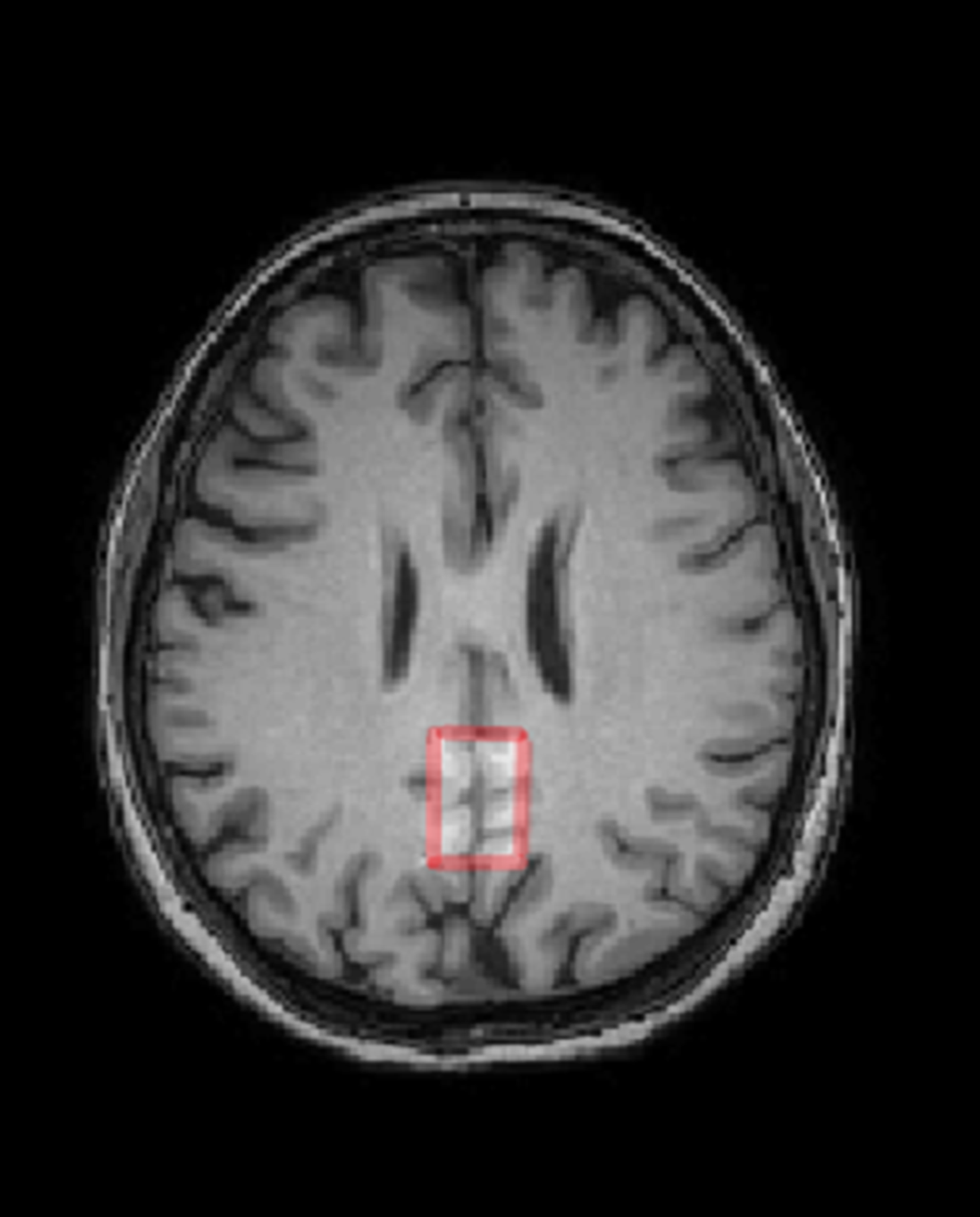 Conclusions
ConclusionsThis study provides insight into neurotransmitter alterations at early-stage schizophrenia. The results demonstrate the region-specific changes in the balance of the main neurotransmitters. Since this balance is crucial for the normal cerebral functioning, the results may facilitate better understanding of the dynamics of the pathological process and provide additional information for understanding the biological mechanisms of the schizophrenia development.
Disclosure of InterestNone Declared
Alterations in brain myelination at early-stage schizophrenia detected by macromolecular proton fraction MRI
- E. Krupina, A. Manzhurtsev, M. Ublinskiy, O. Bozhko, G. Mamedova, V. Ushakov, N. Zakharova, V. Yarnykh, D. Andreyuk, M. Shlyapnikov, G. Kostyuk, T. Akhadov
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S134-S135
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is evidence that cerebral myelination is impaired in schizophrenia. The purpose of this study is to find the myelin content changes in the brain structures of patients with early-stage schizophrenia using the macromolecular proton fraction (MPF) method, and also to evaluate the differences in the myelination of these structures.
ObjectivesTo measure MPF in the brain structures of schizophrenia patients
MethodsForty-five subjects, 22 controls (10m+12f, 31.6±9.7 y.o.) and 23 schizophrenia patients (F20.0, 11m+12f, 31.5±5.1 y.o.). Philips Achieva dStream 3T MRI scanner, standard head coil. The magnetization transfer (TR=20 ms, TE=4.60 ms, FA=10°), T1-weighted (TR=20 ms, TE=4.60 ms, FA=20°) and PD-weighted (TR=20 ms, TE=4.60 ms, FA=4°) were acquired. The MPF maps were reconstructed using home-made software. In FSL, non-brain structures were removed and MPF maps were registered to a standard MNI152 1 mm atlas. Harvard Oxford Cortical and Subcortical atlases were used to select areas of interest. T-test was used in search for between-group differences.
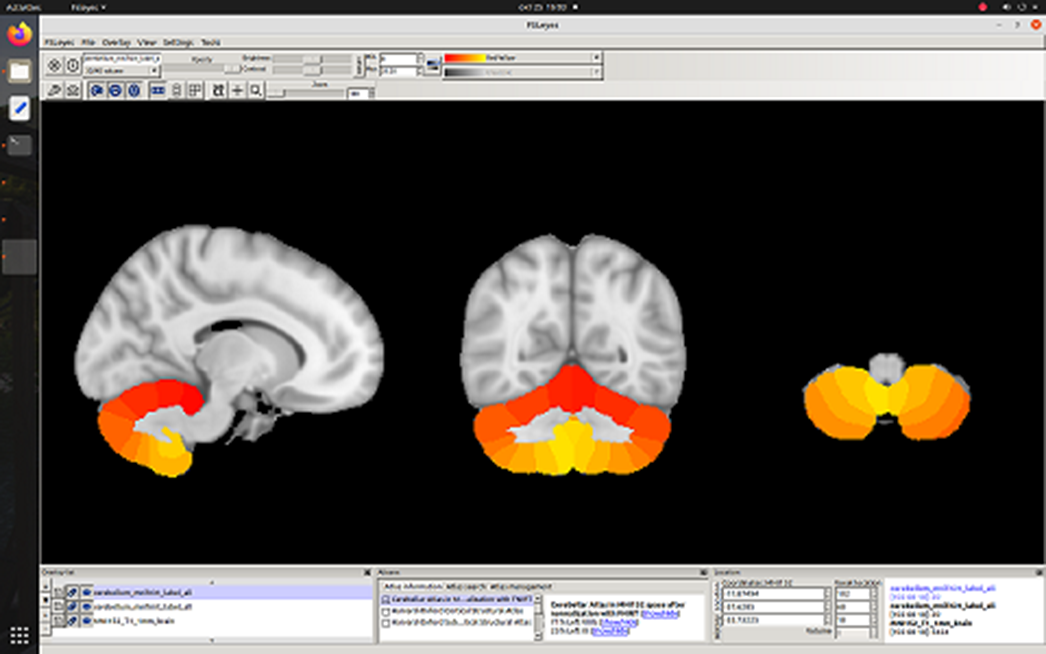
ResultsA 3% decrease in myelination in schizophrenia was observed in whole cerebral cortex p = 0.03) and cerebral white matter (p=0.02). Trends to cortical demyelination were found: paracingular cortex (p=0.06), anterior (p=0.1) and posterior cingulate cortex (p=0.07). No myelination disorders were detected in the cerebellum.
Image:
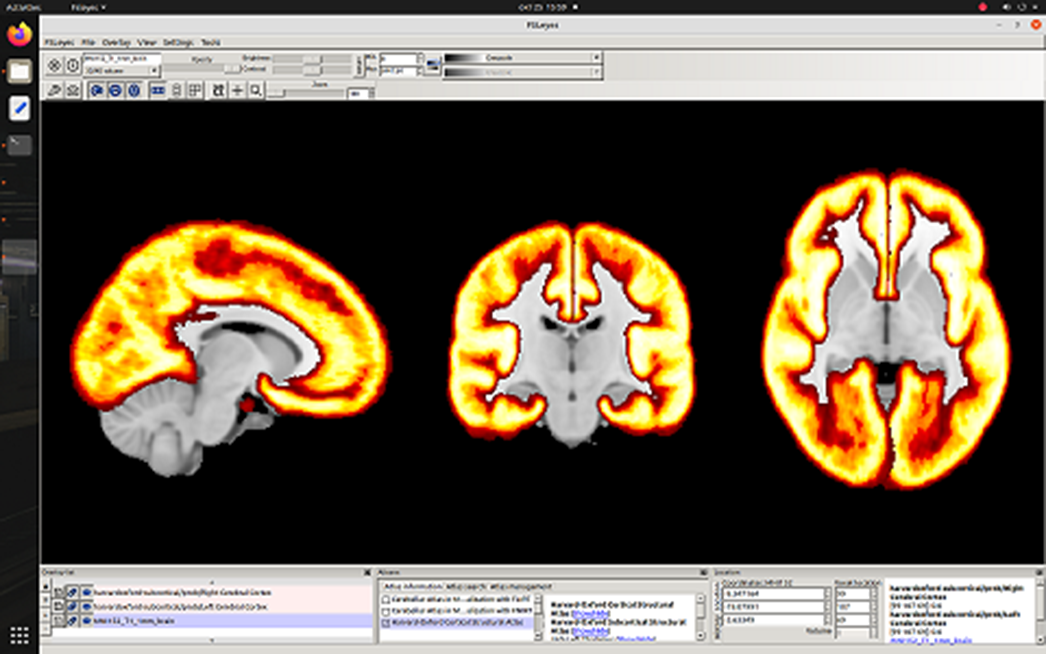
Image 2:
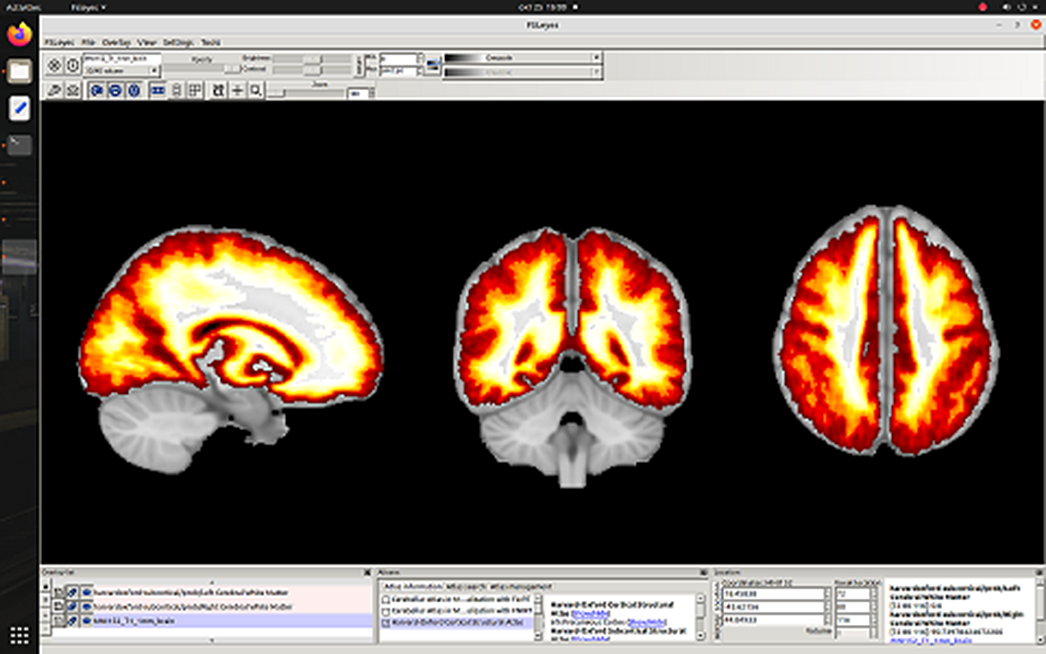
Image 3:
 Conclusions
ConclusionsTo our knowledge, the absence of cerebellar myelination disorders in patients at an early-stage schizophrenia is reported for the first time, while the observed decrease in cerebrum myelination in schizophrenia is consistent with the previous findings. The difference in myelination between cerebellum and cerebrum may help to characterize the dynamics of the pathological process and provide additional information for understanding the biological mechanisms of the development of schizophrenia.
Grant RSF 20-15-00299 (partially).
Disclosure of InterestNone Declared
Attitudes of preoperative cardiac surgery patients toward COVID-19: A cause for concern
- O. Nikolaeva, E. Nikolaev, A. Zakharova, N. Maksimova, E. Litvinova, G. Dulina
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S666-S667
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
During the pandemic, many surveys studied people’s attitude to COVID-19. However, less information is available about the peculiarities of such attitude of the most vulnerable groups including chronic somatic patients who are in need of operative treatment.
ObjectivesTo identify the specificity of preoperative cardiac surgery patients’ attitudes toward COVID-19 as compared to that of healthy people.
MethodsWe used the Attitudes towards COVID-19 questionnaire (Nikolaev E.) to survey 60 preoperative cardiac patients and 327 healthy university students. Difference validity was assessed with significance level of p<0.05.
ResultsCardiac patients are more likely to trust the government measures to fight COVID-19 (t=3.131; p=.002), and their COVID-19-related fears for their life are higher (t=2.793; p=.005). As compared to healthy people, patients are less likely to think that pandemic broke their customary way of life (t=-2.793; p=.005) and plans for the future (t=-3.337; p=.000). Credibly more often than healthy people, cardiac surgery patients consider that it is useless to wear a mask and limit contacts, as any person will eventually catch the virus (t=2.401; p=.017). We did not reveal any more evidently expressed COVID-19-related anxiety in preoperative cardiac surgery patients.
ConclusionsAttitudes of cardiac surgery patients toward COVID-19 manifest in an adequate assessment of threat to their personal health, trust in the government measures, and readiness to change their daily plans. It is latent fatalistic ideas about ultimate uselessness of restrictive measures that pose threat to people’s own health and the health of the people around them, which health professionals should remember in their preventive actions.
DisclosureNo significant relationships.
The structure of depressive manifestations in preoperative cardiac surgery patients
- O. Nikolaeva, E. Nikolaev, N. Maksimova, E. Litvinova, A. Zakharova, G. Dulina
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S691-S692
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
It is common knowledge that depressive disorders are prevalent in cardiac patients. The fact of a prospective heart surgery can have a negative effect on depressive manifestations in cardiac patients.
ObjectivesTo describe representation and structure of depression in preoperative cardiac surgery patients and its correlation with the patients’ personal time perspective
MethodsWe used the Beck Depression Inventory to estimate the level and structure of depression in 60 cardiac surgery patients of both sexes and the Zimbardo Time Perspective Inventory to identify the patients’ personal time perspective.
ResultsWe revealed depression of various manifestations in 53.4% of preoperative cardiac patients; 3.3% of them had severe depression, 11.7% – moderate depression, 8.3% – mild depression, 30.0% – minimal depression. The patients’ average level of depression was certainly higher than the standard one (t=3.295; р=.000). According to degree, the structure of depressive manifestations included asthenia, irritability, sleeping disorders, low sex drive, weight loss, pessimism, tearfulness, difficulty working, and difficulty taking decision. Two patients showed suicidal thoughts. We revealed a positive correlation between the depression level and a Negative-Past time perspective (r=.39) and a negative correlation with the Positive Past time perspective (r=-.27).
ConclusionsWe identified depressive manifestations in every second preoperative cardiac patient. Every sixth one has moderate or severe depression, which calls for special attention. Research in personal time perspective has good prospects for psychological interventions.
DisclosureNo significant relationships.








